Overview
Bariatric surgery encompasses a variety of medical procedures aimed at supporting weight loss by altering how the digestive system works. It is generally recommended for individuals with severe obesity, particularly when conventional methods such as diet, exercise, or weight-loss medications have not led to sustained results.
The primary purpose of these surgeries is to either restrict the amount of food the stomach can store or to reduce the body’s ability to absorb calories and nutrients—sometimes both. Beyond helping with weight reduction, bariatric surgery often contributes to significant improvements in health conditions linked to obesity. These may include type 2 diabetes, high blood pressure, obstructive sleep apnea, and cardiovascular issues. Long-term success depends on lasting lifestyle changes such as healthy eating, consistent physical activity, and regular medical monitoring.
Before undergoing surgery, candidates must go through a comprehensive assessment process. This typically involves physical exams, dietary evaluations, and mental health screenings to ensure they are physically and emotionally prepared for the procedure and the lifestyle adjustments that follow.
In essence, bariatric surgery can offer a transformative opportunity for those struggling with obesity. When combined with a strong personal commitment to healthier living, it can lead to improved overall health, greater mobility, and a better quality of life.
1. What are the types of Bariatric surgery?
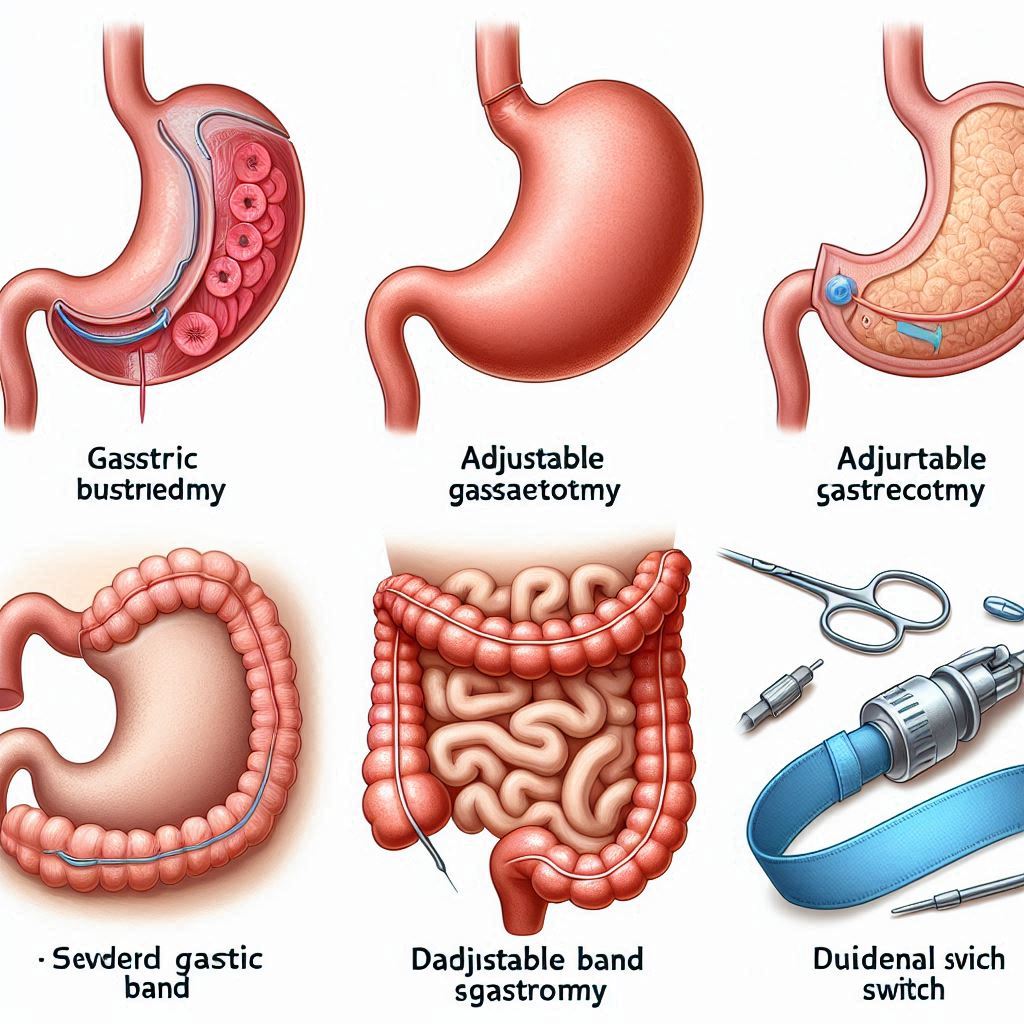
i. Gastric Bypass (Roux-en-Y)
By bypassing a large portion of the stomach and the upper intestine, it limits both food intake and nutrient absorption. It’s highly effective for significant and sustained weight loss.
ii. Sleeve Gastrectomy
In this procedure, a large part of the stomach is surgically removed, leaving a narrow tube or “sleeve.” It reduces the amount of food the stomach can hold and lowers the production of hunger hormones. This helps in both appetite control and weight reduction.
iii. Adjustable Gastric Band (Lap-Band)
The tightness can be adjusted over time. This setup slows food passage and promotes a feeling of fullness with less food. It’s minimally invasive and reversible, but less commonly used today due to lower success rates compared to other options.
iv. Biliopancreatic Diversion with Duodenal Switch (BPD/DS)
This is a two-step surgery: first, a sleeve gastrectomy is performed; second, the small intestine is rerouted to reduce calorie and nutrient absorption drastically. While it’s highly effective for weight loss and metabolic issues, it requires careful lifelong nutritional monitoring.
v. Intragastric Balloon (Non-surgical Option)
It occupies space in the stomach, which helps in reducing food intake. It’s a temporary solution, usually removed after six months, and often used for moderate weight loss goals.
2. Why it is done?

i. To Address Severe Obesity
It’s recommended when a person is significantly overweight (usually with a high BMI) and hasn’t achieved results through diet, exercise, or medication.
ii. To Improve Obesity-Linked Health Problems
It can help reduce or even eliminate health issues such as:
• Type 2 diabetes
• High blood pressure
• Sleep apnea
• High cholesterol
• Joint pain or arthritis
iii. To Lower the Risk of Life-Threatening Conditions
Reduces the chances of heart disease, stroke, and certain cancers associated with long-term obesity.
iv. To Enhance Quality of Life
Many patients experience better mobility, improved self-esteem, and greater participation in daily activities.
v. To Increase Life Expectancy
Significant weight loss can extend life by lowering the risks linked to obesity-related diseases.
vi. To Support Long-Term Weight Control
For people who struggle to maintain weight loss through lifestyle changes alone, surgery provides a more sustainable option.
3. What are the risks?
⚠️ Risks of Bariatric Surgery:
i. Infection
Like any surgical procedure, there’s a chance of developing an infection at the incision sites or inside the body.
ii. Bleeding
Excessive bleeding during or after surgery can occur, requiring medical attention or further treatment.
iii. Blood Clots
There’s a risk of blood clots forming in the legs (deep vein thrombosis) or traveling to the lungs (pulmonary embolism).
iv. Nutritional Deficiencies
Since some surgeries reduce nutrient absorption, patients may develop low levels of vitamins and minerals like B12, iron, calcium, or vitamin D.
v. Digestive Issues
Some people may experience nausea, vomiting, acid reflux, or difficulty digesting certain foods after surgery.
vi. Dumping Syndrome
Eating high-sugar or fatty foods can cause symptoms like dizziness, nausea, or diarrhea shortly after eating — especially after gastric bypass.
vii. Gallstones
Rapid weight loss can lead to the formation of gallstones, sometimes requiring gallbladder removal.
viii. Stomach or Intestinal Leaks
A rare but serious risk where digestive fluids leak through surgical connections, which may need emergency care.
ix. Hernia or Bowel Obstruction
Scar tissue or weakened abdominal muscles may cause hernias or blockages in the intestines.
x. Psychological Effects
Adjusting to body changes and dietary restrictions can lead to mood swings, anxiety, or even depression in some individuals.
| Read more: What is Biohacking? A Beginner’s Guide to Optimizing Your Body |
| The healthy-life-expert.com crew collected the information via a field visit to provide accurate and genuine information. |